Free Shipping PAN India
Dry skin is something that we can all experience at times. It might be due to the weather, central heating or even the clothes we wear. We can experience dry skin on its own or it can be a symptom of a skin condition, such as eczema, psoriasis and ichthyosis.
Healthy skin is usually able to stay hydrated. If the skin barrier is damaged, water is lost from the skin surface, causing dryness. There are many different things that can damage our skin barrier. Knowing what causes your dry skin can help you manage it better, to help maintain healthy skin.
Dry skin can be a problem on its own or it can be a symptom of many other skin conditions. Here are some of the most common conditions.
Dry skin is skin that is lacking in moisture or oils. It can be due to things like the soaps and detergents we use, air conditioning, central heating or the weather. Or it can be a symptom of other skin conditions, such as eczema, psoriasis or ichthyosis.
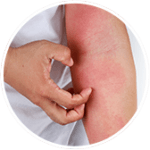
Symptoms of dry skin can vary, depending on how severe it is. In mildly dry skin, you might have rough, slightly scaly skin that is red and may be itchy. Moderately dry skin is more scaly, red, itchy and may feel painful and cracked. With severe dry skin, the itching, scaliness and pain are more intense and any cracks may bleed. The longer you have dry skin, the more severe it may become – and you may find that your skin is often driest on your arms, lower legs and the sides of your stomach. Not everyone has the same skin type, therefore the areas affected is different for everyone.
Dry skin is more likely to become a problem as we age – it affects up to three-quarters of older people aged 64 and over. The condition is also more common in people with certain medical problems, such as an underactive thyroid or kidney failure.
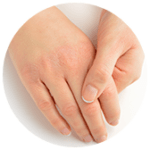
There are many different types of eczema, but the most common is atopic eczema. This is a long-term inflammatory skin problem, also known as atopic dermatitis. Symptoms can be mild, meaning patches of dry skin, occasional itching and maybe some redness. Moderate symptoms include patches of red, dry skin, frequent itching, which can lead to disrupted sleep and confidence. In severe cases, large red areas develop, with dry skin that is always itchy and cracked, which may bleed or ooze. In addition, sleep is often badly disrupted, and so can be other everyday activities.
Although it can affect any part of your body, atopic eczema is most common on your face, scalp, hands and between your body creases like knees, elbows and armpits.
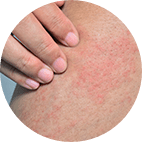
This happens when your skin comes into contact with an allergen that triggers an immune reaction, or with an irritant that removes your skin’s natural protective oils. Skin can suddenly react to a product you’ve been using for a long time without any prior problems. In contact dermatitis, the skin becomes red, dry, flaky and itchy. In severe cases your skin may crack or blister and become weepy.
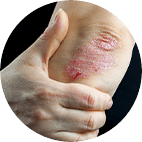
There are many different types of psoriasis, but the most common is plaque psoriasis. Psoriasis can happen at any age, but most often starts between the ages of 10 and 35. It may also be associated with other medical conditions, such as diabetes, heart disease, Crohn’s disease, obesity, anxiety and depression.
There are many different types of ichthyosis, but the most common are ichthyosis vulgaris (which is an inherited condition that usually first develops in babies) and acquired ichthyosis (which develops in adults). Symptoms include fine, white-grey scales (these are said to be ‘fish-like’) which may appear darker on dark-skinned individuals, as well as rough skin, on the arms, legs, torso and scalp. You might find that the skin creases on the palms of your hands and soles of your feet are more pronounced and can sometimes crack. Up to half of people with ichthyosis vulgaris also have atopic eczema symptoms.
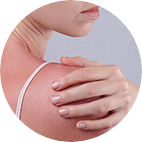
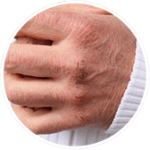


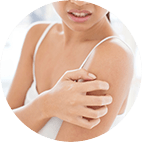
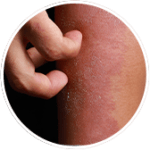

There are many different dry skin triggers, but the following are the most common.
Anything that reduces humidity can lead to dry skin – this includes air conditioning, central heating or wood burners. Dry skin worsens in the winter months because there is less humidity and more chance that the central heating is on.
How to avoid:
Soaps and cleansers are detergents that often have a high pH than our natural skin pH. These can remove water and fats from the skin, damaging our skin barrier. Excessive bathing or showering, especially in hot water, can be bad for skin health.
How to avoid:
Wearing tight clothes can cause dry skin or make it worse. That’s because this type of clothing can rub on the skin, causing friction that leads to dryness.
How to avoid:
In winter, cold weather outside and lack of humidity inside can cause skin dryness. Heat from the summer sun can also dry the skin.
How to avoid:
Stress can make your dry skin worse as it triggers the production of substances in the body that can affect the skin barrier.
How to avoid:
Emollients are moisturizers that can help with dryness and itching. They can come in many forms including creams, lotions, ointments or sprays. Emollients should be applied to the skin regularly, sometimes even multiple times a day. The area of coverage and frequency will change depending on your symptoms and condition, the severity and which product you are using. Having well moisturised skin can help create a barrier which can prevent flare-ups.
Applying emollients regularly can help dry skin by:
Some emollients may contain extra ingredients to help control itchiness.
As regular soaps and cleansers can irritate the skin and cause dryness, it is worthwhile considering using an emollient or a soap substitute when bathing. There are special emollients that can be used for washing just as you would use soap, or you can apply your leave-on emollient as a soap substitute. Be prepared though – while emollient soap substitutes clean effectively, they don’t lather up like regular soap. You can also add emollients to your bath.