Free Shipping PAN India
Did you know that we lose between 30,000 to 40,000 skin cells each day? You usually won’t notice these cells flaking off, so having visibly flaky skin may be a sign that something isn’t quite right.
The outer layer of our skin is known as the epidermis. Normally, this helps trap water to keep our skin moist. Flaky skin can be caused by damage to the epidermis or some other disruption to our usual skin renewal process.
There are many flaky skin triggers, from having a reaction to certain soaps or being in a low humidity environment. It can also be a symptom of other skin conditions such as eczema, psoriasis or ichthyosis.
Flaky skin can be a symptom of many common skin conditions, especially the following.
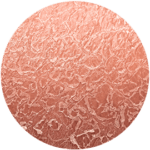
Dry skin is skin that is lacking in moisture or oils, which can result in flaky skin. The seriousness varies; in mildly dry skin, there is light flaking, while in moderately dry skin, there is more flaking. In severe cases, the flaking can be quite drastic. Dry, flaky skin is more common as we get older or if we have certain medical problems such as an underactive thyroid or kidney disease.
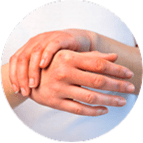
Eczema is a dry, inflammatory skin condition. As eczema skin doesn’t produce as much fat and oils as normal skin, your skin becomes less effective at trapping moisture. There are different types of eczema, many of which can have flaky skin as a symptom. These include:
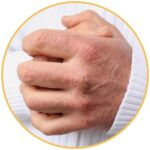
Psoriasis is a type of inflammatory skin condition where the rate at which our skin cells are renewed happens much faster than normal. There are different types of psoriasis that have flaky skin as a common symptom, including:
Ichthyosis is a group of conditions, but the most common types have fine, flaky skin as the main symptom. For some people, ichthyosis is something they inherit from their parents. Others develop it during their life, and more commonly alongside other medical problems such as an underactive thyroid or sarcoidosis, or due to taking certain medicines.
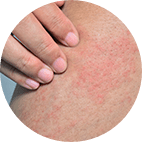
Fungal skin infections can also cause flaky skin. The most common types are those that affect the foot like tinea pedis, better known as athlete’s foot, or those affecting the body such as tinea corporis or ringworm. These are caused by a class of fungus called a dermatophyte. You may have had flaky, itchy or painful skin in the past before you develop the symptoms of fungal skin infections.
Around 70% of us develop athlete’s foot at some point in our lives, particularly during our teenage years. Most people with athlete’s foot have white or red skin with scaly or moist skin between the toes, usually the bit between the two smallest toes. The tell-tale sign of a fungal skin infection on the body is a red and flaky ring around 1-5 cm wide and clear skin in the middle.
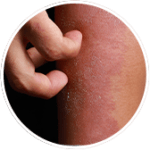
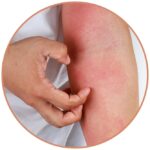
There are many things that can make existing skin conditions worse, causing flaky skin. There are also some factors that can disrupt even healthy skin, making it dry and causing flaking.
Allergens and irritants can trigger reactions, which can lead to flaky skin. Common allergens include the house-dust mite, pet dander, pollen, cosmetics, hair dyes, perfume, plants, medicines and metals such as nickel. Try, where possible, to avoid these triggers.
How to manage:
Soaps and cleansers are detergents that can remove water and fats from the skin, weakening the skin barrier. If you have dry skin, eczema or contact dermatitis, cleansers can make your irritated skin worse.
How to manage:
Wearing tight clothes can cause dry skin or make it worse. Almost half of people with eczema say clothing irritates their skin.
How to manage:
Stress can make dry skin, eczema and psoriasis worse as it triggers the production of substances in your body that can affect the skin barrier.
How to manage:
Anything that reduces humidity can dry skin out – like air conditioning, central heating or wood burners. Some people might find that their skin is drier in the winter months while others with eczema and psoriasis find the sun can help their condition. Hot, humid climates or working in high temperatures are also risk factors for developing athlete’s foot.
How to manage:
It is important to find out what is causing your flaky skin, so you can choose the right treatment. For example, if the problem is a fungal skin infection, a dry skin product won’t be much help. There are many different treatments available to help relieve flaky skin, depending on the underlying cause and how severe it is. If you are unsure or confused about diagnosis, talk to doctor or pharmacist before starting self-treatment.
If your flaky skin is due to dry skin, eczema, contact dermatitis or psoriasis, then using a moisturizer called an emollient can help. You should apply emollients at least twice a day, and in plentiful amounts – even when your skin is clear and feels fine as daily use can prevent flare-ups. However, always check the label of your chosen product to confirm the right way of applying.
Applying emollients regularly can help flaky skin by:
It can also be beneficial to wash with an emollient or soap substitute, as regular soaps and cleansers can irritate the skin and cause dryness. These don’t lather up like regular soap, but still do the job of getting you clean. You can also add emollients to your bath.
Mild steroid creams and ointments can be bought from your pharmacy to help relieve contact dermatitis and mild-to-moderate eczema; majority are safe for use in adults and children aged 10 or over, however always confirm by reading the label. They also help to manage flare-ups in atopic eczema.
Note that steroids should be applied differently to emollients:
If you find that using a mild steroid cream for a week doesn’t bring your skin under control, see your doctor. They’ll be able to discuss a better treatment for your particular situation.
Antihistamines can be used to help relieve severe itch in atopic eczema and contact dermatitis which causes flaky skin. Antihistamines can also be used to help relief allergic symptoms like itchy and flaky skin. Ask your pharmacist or doctor for advice on taking an antihistamine that is right for you.
Antifungal creams and ointments are available to treat athlete’s foot. Some also contain a mild steroid to help reduce any inflammation. You should apply creams to the affected area two or three times a day and use it for at least 2 weeks; or however directed on the label. Sometimes it may be necessary to continue using the cream for more than 4 weeks. If you are using the cream for a foot infection, make sure your feet are washed and thoroughly dried before applying the cream, especially in between the toes. Apply only to the skin and do not use more than the amount recommended. If symptoms do not improve within 7 days, speak to your doctor.
Managing your flaky skin can include using emollients and moisturisers daily, avoiding possible triggers and speaking to your doctor or pharmacist if you’re not sure what is causing your problem.